Abstract
Pulmonary
rehabilitation (PR) is an effective intervention for chronic obstructive
pulmonary disease (COPD). However, uptake of PR is low due to patient frailty,
transportation issues and access. Home-based rehabilitation has been introduced
in recent years to palliate the lack of feasibility for many patients to attend
traditional center-based PR programs. Hence, this study was conducted to
evaluate COPD patients in home-based PR. A total of 56 patients were evaluated
for 6 months’ period in 4 different occasions. It was concluded that home-based
PR was effective as improvement occurred in all parameters.
Keywords: Pulmonary rehabilitation, chronic obstructive
pulmonary disease, noninvasive ventilation
Chronic obstructive pulmonary disease (COPD) is the
third leading cause of mortality worldwide. COPD is a chronic condition for
which patients are using various pharmacological and nonpharmacological
therapies. Pulmonary rehabilitation (PR) is one of the nonpharmacological
therapies1. PR program can be conducted either in facility-based
settings or in home-based settings. PR is an effective intervention for
COPD. However, uptake of PR is low due to patient frailty, transportation
issues, and access2,3. Home-based PR program is mainly offered in
severe COPD and to increase the participation rate of patients. A home-based PR
program is more feasible and convenient, especially for patients with severe
COPD4. Home-based rehabilitation has been introduced in recent years
to palliate the lack of feasibility for many patients to attend traditional
center-based PR programs5,6. Owing to its physiological and
functional effects, PR has been considered unsuitable for older people with
COPD, especially for those at risk of chronic respiratory failure4.
Few studies have evaluated the effectiveness of PR in people with COPD over the
age of 70, in comparison to their younger counterparts. Thus, the main aim of
this study was to evaluate effectiveness of PR in patients who are either older
or younger than 70 years.
This was an observational study conducted in a
private setup offering home-based PR for people with chronic respiratory
disease living in central India, from September 2019 to August 2020 (6-month
enrollment followed by 6-month follow-up assessment). Participants were referred to the home-based PR by their pulmonologist who diagnosed COPD according to the Global Initiative for Chronic Obstructive Lung Disease (GOLD) classification
system
1. Patients who had cardiovascular disease, any contraindication to exercise training, e.g., neurological sequelae and bone and joint diseases, dementia and poorly controlled psychiatric illness, were excluded from study7. Participants
were divided into two groups: one group included individuals aged =70 years, and the other one, people >70 years. The cut-off of 70 years to define the older group was chosen in accordance with the World Health Organization (WHO) report on aging
and health8. All participants signed a written informed consent prior to the start of the program, which included their approval to use the collected data for research purposes.
The rehabilitation team was composed of one nurse,
one physiotherapist, one adapted physical activity instructor, and a weekly
supervised 90-minute home session, for 8 weeks was conducted. The program
included an initial educational needs assessment, endurance physical exercise
training, specific daily living functional task training, strengthening
and balance exercises, lower limb electrostimulation, therapeutic education,
psychosocial support, and motivational communication. Exercise intensity
was progressively adjusted to dyspnea symptoms in order to maintain a score
between 3 and 5 on the Borg 0-10 scale. Apart from the weekly visit of the team
member who supervised the sessions, participants were expected to perform, on
their own, personalized daily physical activities and endurance exercises
training the rest of the week. Patients and team members were instructed to
announce all adverse events, including study withdrawal for any reasons,
hospitalization or death during PR at the 6-month follow-up.
Patients were evaluated at home at the beginning
(M0), at the end of the 2 months PR program (M2) and at 4 months (M4) and
6 months (M6). The 6-minute walk test (6MWT) and the timed up-and-go (TUG) test
were used to evaluate exercise tolerance and functional capacity, respectively.
The psychological status and the health-related quality of life were assessed
with the Hospital Anxiety and Depression (HAD) scale and the Visual Simplified
Respiratory Questionnaire (VSRQ), respectively.
Table 1 is showing baseline
characteristics of patients. From September 2019 to August 2020, total 86
patients were enrolled and referred for home PR. Among them, 14 patients
refused to participate and 16 patients left the study in between the process
and out of these 16 patients, 12 were aged >70 years. Thus, a total of
56 patients completed the study; out of them, 52 were male and 4 were
females. Majority of patients (47) were aged <70 years and remaining (9)
were >70 years. Out of 56 patients, 29 patients had comorbidities and 37
patients were categorized as severe and very severe COPD according to GOLD
guidelines 2019. Among them, 25 patients were current smoker.
Out of total patients, 6 patients were on long-term oxygen therapy
(LTOT) and 3 patients were using noninvasive ventilation (NIV), and all of them
were aged <70 years.
|
Table 1. Baseline Characteristics of Participants
|
|
Characteristics
|
Total group (n = 56)
|
=70 years (n = 47)
|
>70 years (n = 9)
|
P value
|
|
Age (years)
|
63.55 ± 7.9
|
61.28 ± 6.35
|
75.44 ± 2.92
|
0.001
|
|
Male
|
52 (92.9)
|
43 (91.5)
|
9 (100.0)
|
0.364
|
|
Female
|
4 (7.1)
|
4 (8.5)
|
0 (0.0)
|
|
Current smokers
|
25 (44.6)
|
21 (44.7)
|
4 (44.4)
|
0.353
|
|
Ex-smokers
|
23 (41.1)
|
18 (38.3)
|
5 (55.6)
|
|
Nonsmokers
|
8 (14.3)
|
8 (17.0)
|
0 (0.0)
|
|
LTOT
|
6 (10.7)
|
6 (12.8)
|
0 (0.0)
|
0.257
|
|
NIV
|
3 (5.4)
|
3 (6.4)
|
0 (0.0)
|
0.436
|
|
Gold stage
|
|
|
|
|
|
Mild
|
4 (7.1)
|
3 (6.4)
|
1 (11.1)
|
0.693
|
|
Moderate
|
15 (26.8)
|
14 (29.8)
|
1 (11.1)
|
|
Severe
|
27 (48.2)
|
22 (46.8)
|
5 (55.6)
|
|
Very severe
|
10 (17.9)
|
8 (17.0)
|
2 (22.2)
|
|
Comorbidities
|
29 (51.8)
|
21 (44.6)
|
8 (88.8)
|
0.227
|
At baseline, the younger group had lower mean HAD
total score (14.00) as compared to older group (14.56), but it was
statistically nonsignificant (p > 0.05). Anxiety and depression scores were
also lower in younger group than older group, but it was also statistically
nonsignificant (p > 0.05). This means anxiety and depression do not depend on
age of the patient and occur according to the mental condition of the patient.
Similarly, VSRQ and TUG were also better in younger group than older group, but
it was also statistically nonsignificant. This means VSRQ and TUG depend upon
patient’s lung condition and not on the age of the patient. Six-minute step
test (6MST) performance, reflected by mean strokes performed was significantly
better in younger group as compared to older group (337 and 285, respectively)
(Table 2).
|
Table 2. Assessments at Baseline
|
|
Baseline
|
Total group (n = 56)
|
=70 years (n = 47)
|
>70 years (n = 9)
|
T value
|
P value
|
|
HAD
|
14.09 ± 3.53
|
14.00 ± 3.52
|
14.56 ± 3.78
|
0.02
|
0.670
|
|
Anxiety
|
6.41 ± 2.19
|
6.38 ± 2.11
|
6.56 ± 2.74
|
0.51
|
0.831
|
|
Depression
|
7.68 ± 2.29
|
7.62 ± 2.25
|
8.00 ± 2.65
|
1.76
|
0.651
|
|
VSRQ
|
43.86 ± 12.48
|
44.38 ± 12.32
|
41.11 ± 13.67
|
0.42
|
0.476
|
|
6MST
|
311 ± 53
|
337 ± 56
|
285 ± 50
|
2.59
|
0.01
|
|
TUG
|
20.43 ± 5.54
|
20.32 ± 5.58
|
21.00 ± 5.64
|
0.39
|
0.739
|
Table 3 is showing the changes in outcome of PR
from baseline to end of 6 months. Both groups showed improvements in all
outcomes between baseline and M2, M4, and M6. Some of patients (4) from both
groups showed no improvement or even deterioration in M4 and M6 in all
parameters.
|
Table 3. Changes of the Outcomes in M2, M4, M6, after PR
According to Age
|
|
|
=70 years
|
|
>70 years
|
|
M2
|
M4
|
M6
|
M2
|
M4
|
M6
|
|
HAD
|
13.28 ± 3.31
|
12.34 ± 3.01
|
11.62 ± 3.02
|
13.67 ± 3.35
|
12.89 ± 3.41
|
11.56 ± 2.96
|
|
Anxiety
|
5.89 ± 1.51
|
5.81 ± 1.47
|
5.47 ± 1.54
|
5.89 ± 1.54
|
5.44 ± 1.34
|
5.33 ± 1.58
|
|
Depression
|
7.38 ± 2.41
|
6.53 ± 1.96
|
6.15 ± 1.67
|
7.78 ± 2.64
|
7.44 ± 2.51
|
6.00 ± 1.50
|
|
VSRQ
|
51.21 ± 9.89
|
57.89 ± 7.23
|
64.89 ± 4.65
|
50.67 ± 11.49
|
57.67 ± 8.81
|
64.11 ± 5.28
|
|
6MST
|
406 ± 65
|
409 ± 86
|
448 ± 88
|
302 ± 56
|
309 ± 74
|
328 ± 98
|
|
TUG
|
17.91 ± 5.07
|
14.45 ± 3.65
|
11.55 ± 2.61
|
18.56 ± 4.91
|
15.22 ± 4.05
|
12.22 ± 3.15
|
|
|
|
|
|
|
|
|
Figure 1 is showing decreasing
mean of total HAD score in both age groups at 2, 4, and end of 6 months and
fall of HAD score was more in >70 age group (p > 0.05). Figures
2 and 3 are showing improvement in anxiety and depression scores individually
at 2, 4, and end of 6 months of PR. More improvement in anxiety was seen
in older age group than younger age group (p > 0.05). Similarly, more
improvement in depression was seen in older age group than younger age group (p
> 0.05).
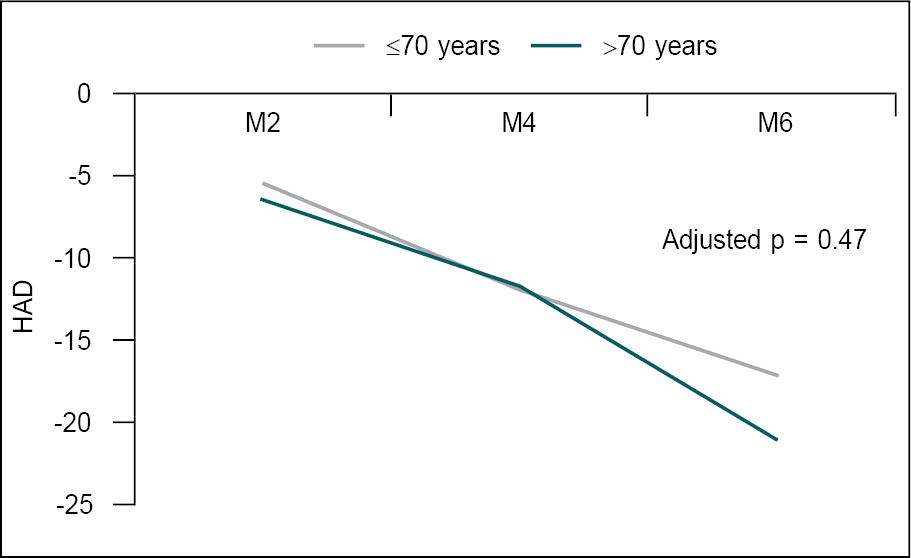
Figure 1. Mean total HAD score in both age groups at M2, M4, and M6.
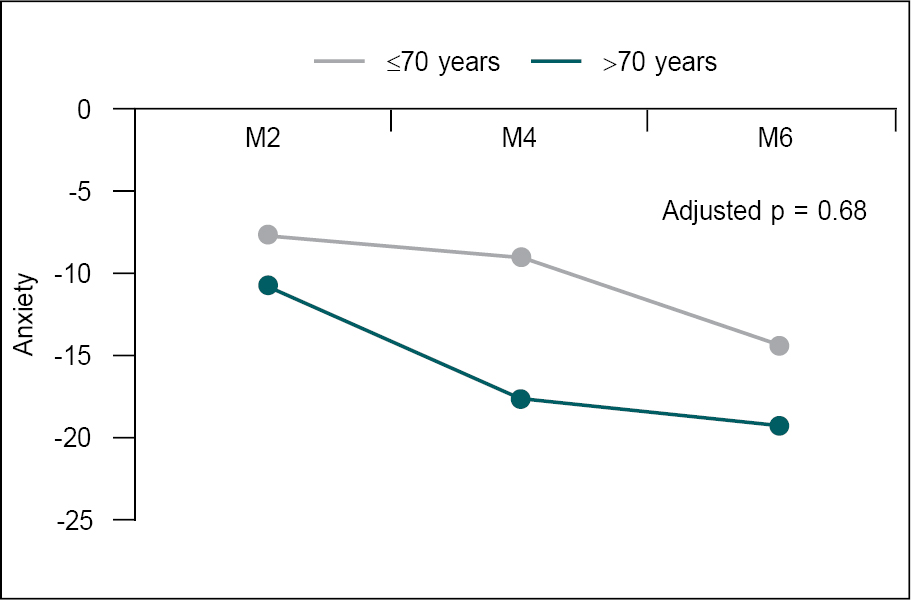
Figure 2. Change in anxiety score at M2, M4 and M6.
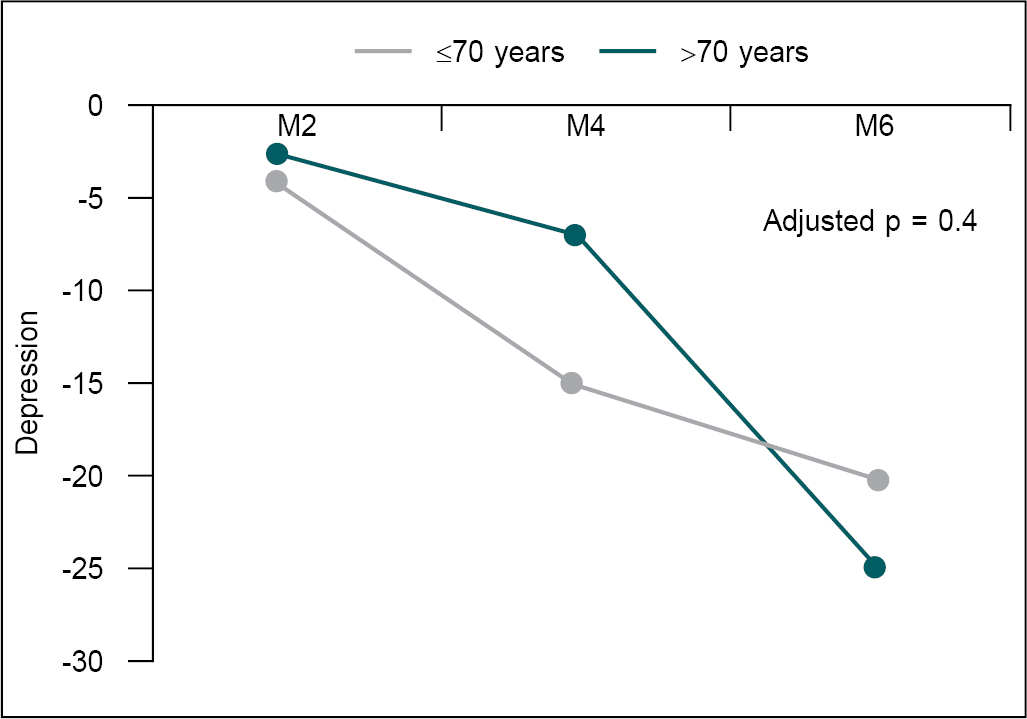
Figure 3. Change in depression score at M2, M4, and M6.
Figure 4 is showing increasing mean of VSRQ scale
in both age groups, which means improvement in respiratory conditions of
patients occurred in both groups (p > 0.05).
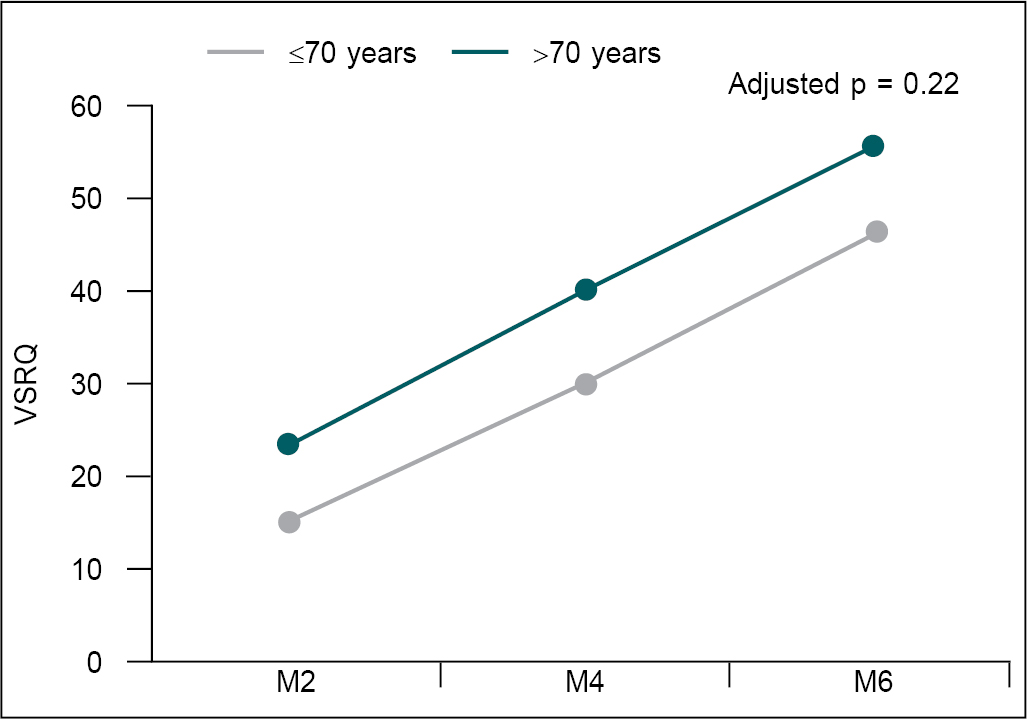
Figure 4. Change in VSRQ at M2, M4, and M6.
Figure 5 is showing increase of 6MST in both groups
which indicates the mean number of strokes increased in both age groups and
increment was more in younger age group than older age group (p > 0.05).
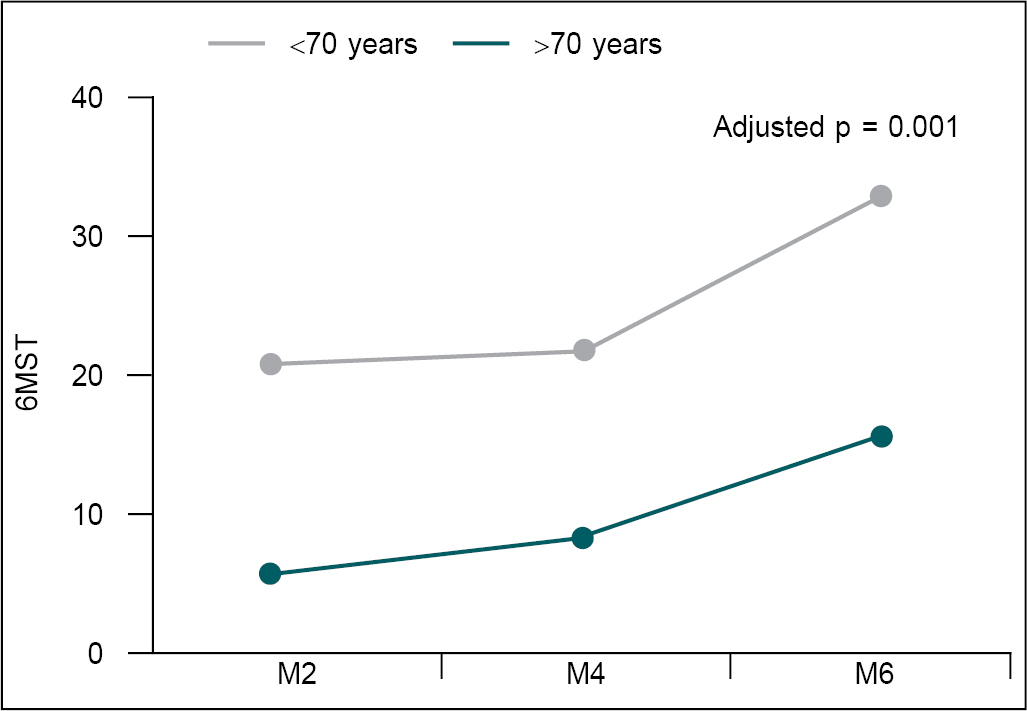
Figure 5. Change in 6MST at M2, M4, and M6.
Figure 6 is showing decrease of TUG in both groups,
which means the mean time of patient performing TUG became less from baseline
to 6 months (p > 0.05).
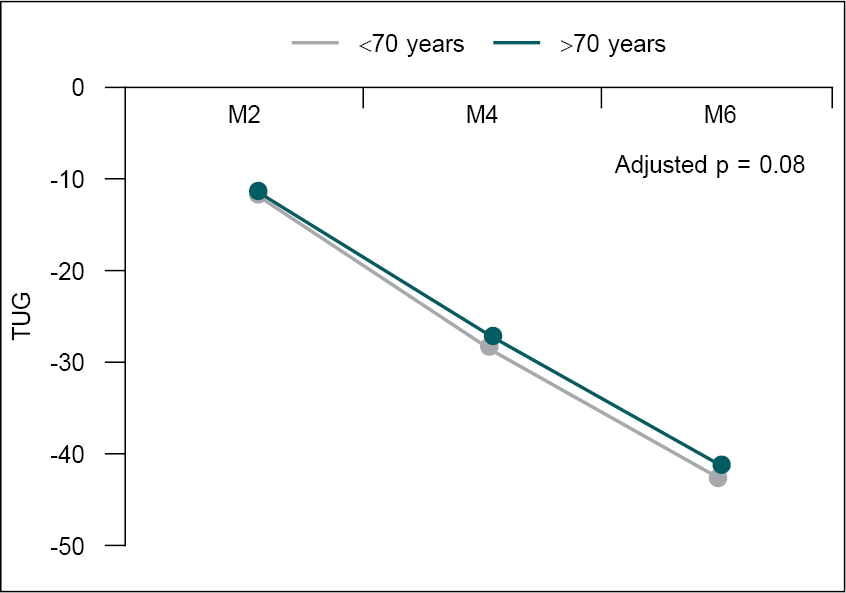
Figure 6. Change in TUG at M2, M4, and M6.
The purpose of this study was to observe the
effectiveness of home-based PR program at 2, 4, and end of 6 months.
Patients were categorized in two groups: age =70
years (younger) and >70 years (older). Out of 56 patients, 47 were in
younger and remaining 9 patients were in older group. Dropouts and failure to
program are common problems in older patients. In this study, less number of
patients were there in older group. This was one of the drawbacks of this
study. Out of 16 patients who left the study in between, 12 patients were from
older group. Out of total patients, 25 (44.6%) patients were current smoker, 21
patients were from younger group and 4 patients were from older group.
Smoking cessation was also prescribed before and during program as smoking can
reduce fitness and the ability to perform exercises9. In this study,
almost half (48.2%) of patients had severe COPD and remaining patients had mild
(7.1%), moderate (26.8%), and very severe (17.9%) COPD. Korkmaz Ekren et al did
a study and found benefits from PR for mild to moderate COPD and suggested that
these patients should be included in PR10.
At baseline all scores were towards better side in
younger group than older group, but they were not comparable, p value was not
significant except 6MST parameter, which means younger patients attained more
number of strokes than older patients. Anxiety and depression were also
less in younger group than older group. A study was conducted by Gephine et al
and they observed that anxiety component was high in younger group and
depression component was same in both groups. Similarly, VSRQ was also
comparable in both groups and TUG was higher in older group4.
In our study, the number of patients was very less in older group. This may
explain the above differences.
In our study, from baseline to end of program,
improvement occurred in all parameters in both groups and more improvement
occurred in total HAD score, anxiety, and depression in older group. According
to the study of Gephine et al, improvement was seen in all parameters in
younger group but in older group improvement was present in all parameters up
to initial 2 months from baseline and thereafter improvement was seen only in total
HAD score, anxiety component and depression4. In our study,
improvement in all parameters was comparable in both groups except 6MST
strokes, which was lesser in older group. This difference could be due to
higher age as exercise tolerance and fitness are reduced in elder persons as
compared to younger individuals.
This study concluded that home-based PR was
effective as improvement occurred in all parameters and improvement was
significant in 6MST strokes from baseline to end of 6-month of program.
1.
Global Initiative for Chronic
Obstructive Lung Disease, global strategy for the diagnosis, management, and
prevention of chronic obstructive pulmonary disease-revised, GOLD online 2019.
Available at: http//www.goldcopd.org
2.
Spruit MA, Singh SJ, Garvey C, ZuWallack R, Nici L,
Rochester C, et al; ATS/ERS Task Force on Pulmonary Rehabilitation. An official
American Thoracic Society/European Respiratory Society statement: key concepts
and advances in pulmonary rehabilitation. Am J Respir Crit Care Med.
2013;188(8):e13-64.
3.
Keating A, Lee A, Holland A. What
prevents people with chronic obstructive pulmonary disease from attending
pulmonary rehabilitation? A systematic review. Chron Respir
Dis. 2011;8(2):89-99.
4.
Gephine S, Le Rouzic O, Machuron F, Wallaert B,
Chenivesse C, Saey D, et al. Long-term effectiveness of a home-based pulmonary
rehabilitation in older people with chronic obstructive pulmonary disease: a
retrospective study. Int J Chron Obstruct Pulmon Dis. 2020;15:2505-14.
5.
Holland A. Telehealth reduces hospital
admission rates in patients with COPD. J Physiother. 2013;59(2):129.
6.
Holland AE, Hill CJ, Rochford P, Fiore J, Berlowitz
DJ, McDonald CF. Telerehabilitation for people with chronic obstructive pulmonary
disease: feasibility of a simple, real time model of supervised exercise
training. J Telemed Telecare. 2013;19(4):222-6.
7.
Kallianos A, Charikiopoulou M, Arapis I, Velentza
L, Kokkolios A, Bletsa M, et al. The impact of comorbidities on pulmonary rehabilitation
outcomes in patients with COPD. Euro Respir J. 2016;48(Suppl 60):PA3790.
8.
World Health Organisation. WHO report on ageing,
WHO online; 2015. Available at: https://apps.who.int/iris/bitstream/handle/10665/186463/9789240694811_eng.pdf;jsessionid=16C999C7FBB4BC5A734D1997150EFCDE?sequence=1
9.
Mesquita R, Gonçalves CG, Hayashi D, Costa Vde S,
Teixeira Dde C, de Feritas ERFS, et al. Smoking status and its relationship
with exercise capacity, physical activity in daily life and quality of life in
physically independent, elderly individuals. Physiotherapy. 2015;101(1):55-61.
10.
Korkmaz
Ekren P, Gürgün A, Elmas Uysal F, Tuncel S, Deniz S, Karapolat H, et al.
Effects of pulmonary rehabilitation in patients with mild-to-moderate chronic
obstructive pulmonary disease: Bottom of an iceberg. Turk J Phys Med Rehabil.
2018;64(2):162-9.