Herpes
zoster (HZ) as well as varicella are caused by varicella-zoster virus. It is
uncommon in children. Cases have been reported in literature among all ages
from neonate to old age. We report this case of HZ ophthalmicus in a healthy
child born to healthy mother with a history of varicella infection in the third
trimester (7th month of gestation). Early diagnosis and treatment reduce
complications. Preconceptional varicella-zoster vaccine is also a matter of concern.
Keywords: Herpes zoster ophthalmicus, infant,
varicella-zoster vaccine, varicella-zoster
Herpes zoster (HZ) and varicella are caused by the
same virus, i.e., varicella-zoster virus1. Cases have been reported
in medical literature from neonates to old age, but it is rare in
immunocompetent children. Overall incidence of HZ is 3.4/1,000 people, whereas
in children in the age group of 0 to 9 years and 10 to 19 years it is 0.74 and
1.38, respectively2. Herpes zoster ophthalmicus (HZO) is caused by
varicella-zoster virus 3, i.e., human herpes virus 3.
Presented here is the case of a 13-month-old baby
with HZO.
A 13-month-old, 7.5 kg, female child, born
full-term, normal vaginal delivery, was brought with vesicular eruptions over
right side of forehead, erythema, and swelling over right upper eyelid since 4
days. It was accompanied with photophobia and watery discharge from the right
eye. Cutaneous examination revealed multiple, tense, grouped vesicular lesions
with erosions and yellow crust on erythematous base present over scalp,
forehead extending to right periorbital region, nasal bridge, and tip of nose
(Fig. 1), suggesting involvement of nasociliary branch of the ophthalmic
division of right trigeminal nerve, thus positive Hutchinson’s sign. There was
marked erythema and swelling of the right upper eyelid with difficulty in
opening of right eye.
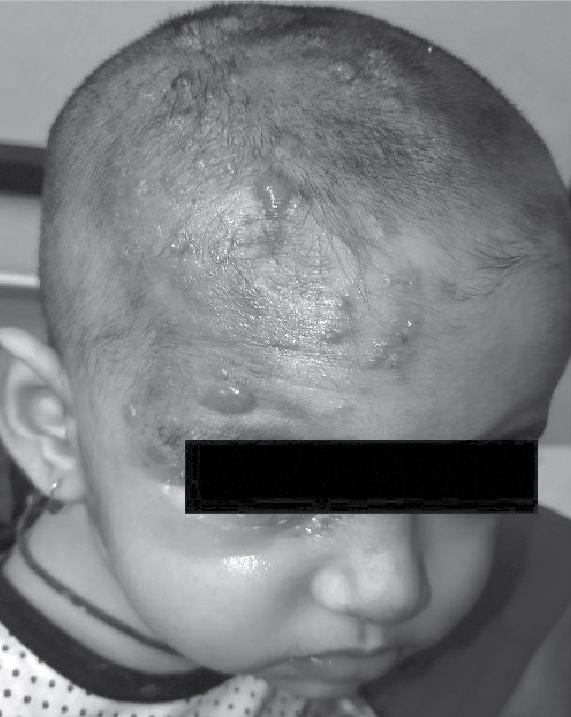
Figure 1. Vesicular eruption over right side of forehead, nose and tip of nose with marked erythema and swelling of right upper eyelid.
On ophthalmic consultation, tobramycin eye drop
twice and lubricating eye drop four times a day were started. Visual acuity was
difficult to assess. Left eye was normal. There was no past history of
varicella in the infant and neither was she vaccinated for varicella. Her
mother had developed varicella infection during 7th month of gestation and was
treated with tablet acyclovir five times a day for 7 days with other
symptomatic drugs. Systemic examination and developmental milestones of the
child were assessed by pediatrician and were normal. Child was irritable and
so, was admitted. Treatment with injection acyclovir 75 mg intravenously three
times a day for 7 days was initiated. Antibiotics were started to combat
secondary bacterial superinfection. Topical mupirocin ointment and acyclovir
eye drops were also added. Giemsa stained Tzanck smear showed presence of
multinucleated giant cells, an epithelial cell containing numerous nuclei (Fig.
2A). Papanicolaou stained smear from scraping showed presence of acantholytic
cells (Fig. 2B). Parents and child were also screened for human
immunodeficiency virus (HIV) and both of them along with child came nonreactive
for both HIV type I and II. Symptoms subsided remarkably within 1 week of
treatment (Fig. 3). Right eye showed hyperemic conjunctiva with no other signs
of ocular involvement.
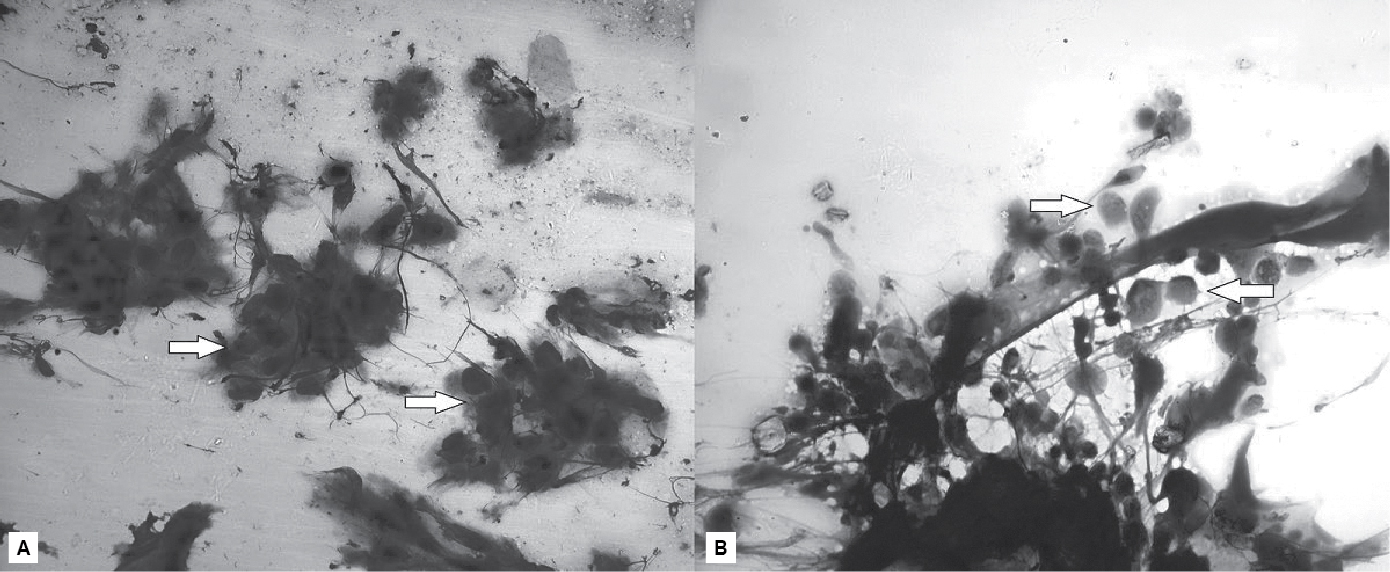
Figure 2. Smear
showing presence of multinucleated giant cells (white arrow) (Giemsa, x400) (A)
and acantholytic cells (white arrow) (PAP, x400) (B).
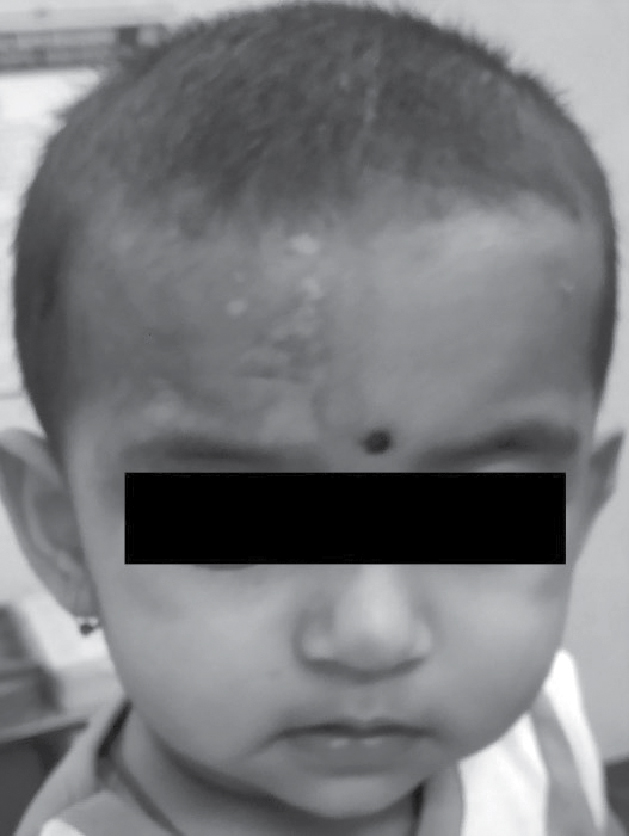
Figure 3. Complete resolution after 1 week of treatment.
Herpes virus is a neurotropic virus3.HZ occurs more commonly in elderly patients but is rare in childhood4.
It has milder course with less residual damage in children than adults5.Varicella-zoster virus is responsible for both varicella and HZ1.
Once a person suffers from varicella infection, the virus remains dormant in
dorsal ganglion of spinal nerve root of spinal cord2.As
immunity decreases, these virus reactivate to produce HZ2. If mother
suffers from varicella infection in second-half of pregnancy, then there are
higher chances of the child suffering from HZ in 1st year of life6.Similar observation was seen in our case. Infantile HZ is due to
intrauterine infection of varicella-zoster virus than postnatal6.Generally HZ occurs in children with immunodeficiency like malignancy or
HIV infection, but it can also occur in immunocompetent individuals5.HZ affects eye in 10%-20% cases4.
Hutchinson’s sign is presence of vesicles on
tip/side of nose which indicate involvement of nasociliary nerve of ophthalmic
division of trigeminal nerve7. If Hutchinson’s sign is positive, it
means sight-threatening ocular changes can occur8.In our
case, there was involvement of tip of nose.
In our case, there was history of maternal
infection of varicella at the 28th week of gestation. Maternal varicella before
28 weeks of gestation increases chances of congenital varicella syndrome (CVS)
in newborn and risk is negligible after 28 weeks of gestation. CVS includes
multiple developmental defects like microcephaly, hydrocephaly, aplasia of
brain, limb hypoplasia, Horner’s syndrome, etc. In our case, mother suffered
from varicella at 28 weeks of gestation; hence newborn did not suffer from CVS.
In our case, fetus was exposed to varicella in
third trimester in intrauterine life but child developed HZO without developing
clinical symptoms of varicella due to the presence of maternal antibody. This
is similar to case reported by Van Aelst et al in a 2.5-year-old child9.
Varicella vaccine is live attenuated vaccine; so
contraindicated in pregnancy and immunocompromised patients, but it can be
given prior to conception.10 Two doses are given 1 month apart. In
our case, the mother had no history of varicella in past and there are no
studies in literature where such cases are to be vaccinated with varicella
vaccine before planning for pregnancy.
There are only few published reports on HZ ophthalmicus
in immunocompetent children in Indian literature. We are reporting this case as
rare pediatric case of HZO in an immunocompetent infant. This case report
demonstrates that HZ ophthalmicus can occur in an immunocompetent child with a
history of varicella infection to mother during late gestational months. Early
diagnosis and treatment decrease fatal complications. Also, preconception
vaccination of females not exposed to varicella-zoster virus in past is a
matter of concern.
1.
Weller TH. Serial propagation in vitro of agents
producing inclusion bodies derived from varicella and herpes zoster. Proc Soc
Exp Biol Med. 1953;83(2):340-6.
2.
Hope-Simpson RE. The nature of herpes zoster: a
long-term study and a new hypothesis. Proc R Soc Med. 1965;58(1):9-20.
3.
Savage MO, Moosa A, Gordon RR. Maternal varicella
infection as a cause of fetal malformations. Lancet. 1973;1(7799):352-4.
4.
Ragozzino MW, Melton LJ 3rd, Kurland LT, Chu CP,
Perry HO. Population-based study of herpes zoster and its sequelae. Medicine
(Baltimore). 1982;61(5):310-6.
5.
Liesegang TJ. Herpes zoster ophthalmicus natural
history, risk factors, clinical presentation, and morbidity. Ophthalmology.
2008;115(2 Suppl):S3-12.
6.
Enders G, Miller E, Cradock-Watson J, Bolley I,
Ridehalgh M. Consequences of varicella and herpes zoster in pregnancy:
prospective study of 1739 cases. Lancet. 1994;343(8912):1548-51.
7.
Frary J, Petersen PT, Pareek M. Hutchinson’s sign
of ophthalmic zoster. Clin Case Rep. 2019;8(1):219-20.
8.
Zaal MJ, Völker-Dieben HJ, D’Amaro J. Prognostic
value of Hutchinson’s sign in acute herpes zoster ophthalmicus. Graefes Arch
Clin Exp Ophthalmol. 2003;241(3):187-91.
9.
Van Aelst S, Winters L, Janssen K, Laffut W,
Thibaut K. A healthy 2.5-year-old boy with herpes zoster ophthalmicus as
primary presentation. J Pediatric Infect Dis Soc. 2015;4(4):e160-2.
10.
Centers
for Disease Control and Prevention. Morbidity and Mortality Weekly Report
Prevention of Varicella Recommendations of the Advisory Committee on
Immunization Practices (ACIP). Morb Mortal Wkly Rep Recomm. 2007;56(4):7.