Abstract
Mullerian duct anomalies
(MDAs) are congenital anatomic abnormalities of the female genital tract that
arise from non-development or nonfusion of the mullerian ducts or failed
resorption of the uterine septum, with a reported incidence of 0.1%-10.0%. MDAs
are clinically important because they are associated with an increased
incidence of impaired fertility, menstrual disorders, and obstetric
complications. We hereby report a case of a primigravida with full-term
pregnancy with obstructed labor referred from a primary health center. During
the course of examination, she was found to have congenital abnormality of
uterus and vagina. She underwent an emergency cesarean section with good
perinatal outcome. Women with uterus didelphys belong to a high-risk group,
although pregnancy outcome is comparatively good.
Keywords: Mullerian duct anomalies, congenital anatomic
abnormalities, obstructed labor, uterus didelphys
The true incidence of congenital uterine anomalies
in the general population and among women with recurrent pregnancy loss is not
known accurately. Although incidences of 0.1%-10.0% have been reported, the
overall data suggest an incidence of 1% in the general population and 3% in
women with recurrent pregnancy loss and poor reproductive outcome. Female
genital tract develops from 3 sites, ovaries from the germ cells that migrate
from the yolk sac into the mesenchyme of the peritoneal cavity and develop into
ova and supporting cells; lower third of vagina develops from the ascending
sinovaginal bulb; and uterus, fallopian tubes and upper two-thirds of vagina
develop from the fusion of two mullerian ducts. Incomplete fusion of the
mullerian or paramesonephric ducts results in the most common types of uterine
malformation: uterus didelphys, uterus bicornis bicollis, uterus bicornis
unicollis, uterus subseptate, uterus arcuatus, and uterus unicornis. Uterus
bicornis bicollisis characterized by double or single vagina,
double cervix and two single-horned uterus which s how partial fusing of their muscular walls with duplication running right down to the uterine orifice. Congenital anomaly of the mullerian duct system
can result in various urogenital anomalies including uterus didelphys with blind hemivagina and ipsilateral renal agenesis1.
The diagnosis of this condition is usually made
after menarche, but its rarity and variable clinical features may contribute to
a diagnostic delay for years after menarche2. With timely and
accurate diagnosis, appropriate management is likely to provide the best
possible outcome for all such patients.
A 20-year-old primigravida, wife of a farmer, who
was referred from a primary health care center, reported to labor room on 31st
May 2009 at 09:13 pm with a history of 9 months of amenorrhea and leak per
vagina since 3 days and pain abdomen since 3 days. She was married for 1
year.
General examination was unremarkable.
On abdominal examination, uterus was term size and cephalic
presentation and there was an unusual contour of abdomen on right side. Fetal
heart sound was localized in the right iliac fossa and was 146 bt/min. Per
speculum examination revealed complete vertical vaginal septum (Fig. 1) and
bulging of vaginal fornices in right hemivagina, active clear liquor leak
demonstrated on the blade of speculum in right hemivagina. Internal examination
revealed right cervix was partially effaced and 2 cm dilated and presenting
part at minus three station, and in left hemivagina cervix was uneffaced and os
closed.

Figure 1. Per speculum examination showing right and left hemivagina with complete vertical vaginal septum.
On clinical examination, the
pelvis was found to be grossly contracted. A decision for emergency cesarean
section was made. She underwent an emergency cesarean section on 01/06/09 at
12:30 am; a full-term male baby of weight 3.2 kg was extracted who cried after
delivery. Uterus was found to be bicornis bicollis and pregnancy was found in
the right hemi-uterus (Figs. 2 and 3). Postoperative stay was uneventful and
sutures were removed on 7th postoperative day and the patient was discharged
the same day.
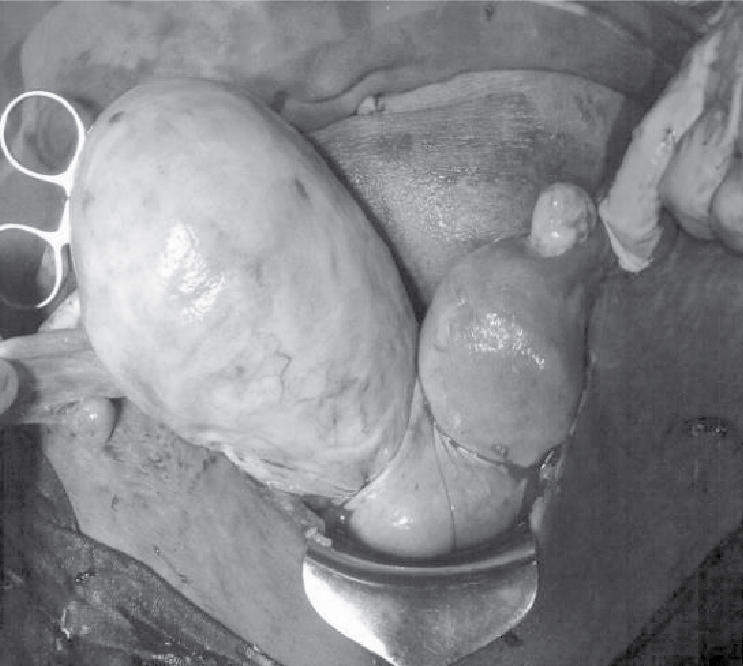
Figure 2. Anterior view of gravid right hemi-uterus with incision on the lower segment and
nongravid left hemi-uterus.
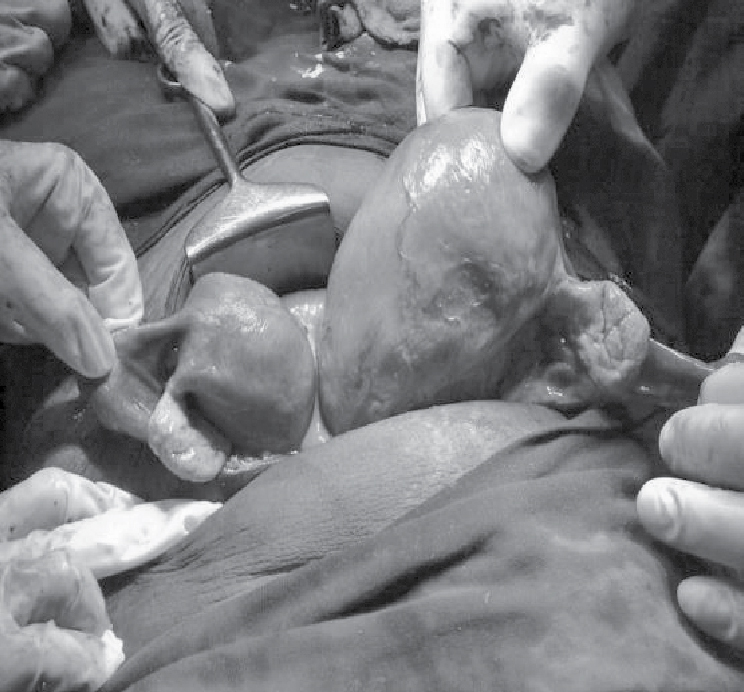
Figure 3. Posterior view of didelphic gravid hemi-uterus.
Mullerian anomaly rate is
reported between 0.1% and 1% in general population with significantly higher
rates associated with infertility and reproductive wastage. Uterus didelphys is
one of the least common anomalies, representing approximately 5%-7% of
müllerian defects. The reproductive outcomes are slightly better than those of
women with unicornuate uterus. Acién reported that poorest viability results
were found in the bicornuate (40%), arcuate (45%), and septate uterus groups
(59%), and rates of children surviving for more than 7 days were around 70% in
the bicornis bicollis, didelphys, unicornuate, and subseptus uterus groups3.Maneschi et al reported live birth rate of 81% and suggested that
reproductive and gestational performances of women with uterus didelphys are
preserved. In patients with infertility complaints, associated causes must be
ruled out before surgical correction. If these are present, their correction
must be attempted as first therapeutic step, and term pregnancy with live baby
is the rule4. Interestingly, pregnancy has been observed
consistently in right horn5.
In case of single pregnancy,
it is in the right uterus in uterus didelphys. Even in this present case,
pregnancy has been found in the right hemi-uterus. Heinonen and colleagues
observed a cesarean section rate of 82% and fetal survival rate of 67.5% and
premature delivery of 21%6.All the patients also had a
longitudinal vaginal septum.
Three-dimensional sonography has contributed the
most and has become the investigation of choice in units where available. Raga
et al and Wu et al reported that three-dimensional sonography offered a 100%
specificity and is reproducible and reliable noninvasive diagnostic procedure
for the exclusion of uterine anomalies and was able to differentiate between
the different anomalies7,8. Magnetic resonance imaging (MRI) is the
most sensitive imaging modality for congenital anomalies.
Congenital uterovaginal anomalies can have adverse
effects on pregnancy outcome. Early diagnosis and an aggressive evaluation of
any patient presenting with mid-trimester abortion, premature labor, malpresentation,
prevent additional pregnancy wastage, and maternal morbidity and are likely to
provide the best possible outcome for all such patients.
1.
Zurawin RK, Dietrich JE, Heard MJ, Edwards CL. Didelphic uterus and
obstructed hemivagina with renal agenesis: case report and review of the
literature.J Pediatr Adolesc Gynecol. 2004;17(2):137-41.
2.
Varras M, Akrivis Ch, Karadaglis S, Tsoukalos G,
Plis Ch, Ladopoulos I. Uterus didelphys with blind hemivagina and ipsilateral renal agenesis
complicated by pyocolpos and presenting as acute abdomen 11 years after
menarche: presentation of a rare case with review of the literature.Clin Exp Obstet Gynecol. 2008;35(2):156-60.
3.
Acién P. Reproductive performance of women with uterine malformations.Hum Reprod. 1993;8(1):122-6.
4.
Maneschi I, Maneschi F, Parlato M, Fucà G,
Incandela S. Reproductive performance in women with uterus didelphys.Acta Eur Fertil. 1989;20(3):121-4.
5.
Suhail S, Suhail MF, Khan H. Uterus didelphys - a
case having pregnancy only in her right uterus. 2007.
6.
Heinonen PK. Uterus didelphys: a report of 26
cases. Eur J Obstet Gynecol Reprod Biol. 1984;17(5):345-50.
7.
Raga F, Bonilla-Musoles F, Blanes
J, Osborne NG. Congenital Müllerian anomalies: diagnostic accuracy of
three-dimensional ultrasound. Fertil Steril. 1996;65(3):523-8.
8.
Wu MH, Hsu CC, Huang KE. Detection of congenital
müllerian duct anomalies using three-dimensional ultrasound. J Clin Ultrasound. 1997;25(9):487-92.