Abstract
Objective: To evaluate retrospectively the efficacy of ultrasound-guided embryo transfer method on pregnancy and implantation rate and compare with clinical touch method. Material and methods: The results of 582 cycles from our in vitro fertilization
and embryo transfer (IVF-ET) program conducted at Jaipur Fertility Centre, an Infertility Unit of Mahatma Gandhi University of Medical Sciences and Technology, Jaipur, Rajasthan were analyzed retrospectively and comparison was made between those carried
out using ultrasound guidance and those by clinical touch method. Results: Higher pregnancy and implantation rates (37.19% and 19.66%, respectively) were found in the group using the transabdominal ultrasound guidance during ET compared with those
in the group using the clinical touch method (30.92% and 16.22%, respectively). The difference was not statistically significant. Conclusion: Older women (>35 years) and in the subgroup when the clinician rated the transfer procedure as easy with
some difficulty, there appeared to be a substantial improvement in the pregnancy rate and the difference was statistically significant. We believe that ultrasound-guided ET should be used in these subgroups.
Keywords: Clinical touch,embryo transfer, in vitro fertilization, retrospective study, ultrasound-guided, air bubble
Transabdominal ultrasound-guided embryo transfer (ET) has been described by various authors since 1985 to improve the pregnancy rate1-4. However, significantly higher pregnancy rates following transabdominal ultrasound guidance have not been
consistently demonstrated. Lindheim et al, first reported that ultrasound guidance improved pregnancy outcome only in easy transfer5. Subsequently, two studies demonstrated significant differences between the clinical touch method and transabdominal
ultrasound-guided ET retrospectively6 and prospectively
7.
Most studies trying to address the issue of whether ultrasound guidance is beneficial to ET conclude that although pregnancy rates may not be significantly raised, ultrasound guidance provides both the clinicians and patients with greater degree of confidence
in the ET procedure3,4,8.We divided our study population according to: i) Number of embryo transferred; ii) age of patient; and iii) ease of transfer to delineate a subgroup of patients that would particularly benefit from their embryo
being transferred under ultrasound guidance.
Material and Methods
A retrospective study of in vitro fertilization and embryo transfer (IVF-ET) cycles from June 2011 to August 2012 was performed. Between June 2011 to December 2011 the clinical touch method had been adopted for 262 cycles in our IVF-ET program.
Between January 2012 and August 2012, 320 cycles of IVF-ET were performed under transabdominal ultrasound guidance. During both periods, there was no change in ovarian stimulation method, oocyte retrieval, culture media and culture system. For ET,
Wallace and Cook echo tip catheters were used. Exclusion criteria were: age 45-year-old, more than three previous assisted conception cycles and transfer requiring general anesthesia for the patients. One clinician and three ultrasonographers
were involved in the study. All ultrasonographers were specialists in infertility. An ultrasound machine with 3.75 MHz transabdominal probe was used on all women in ultrasound group.
Controlled ovarian hyperstimulation (COH) was carried out in more than 85% of patients with recombinant follicle-stimulating hormone (FSH) and human menopausal gonadotropin (hMG) with half-dose of gonadotrophin-releasing hormone (GnRH) agonist after down
regulation with GnRH agonist in the preceding late luteal phase. Rest of the patients were induced by short protocol with GnRH agonist along with recombinant FSH or hMG. Follicular growth was followed by transvaginal ultrasonography and once adequate
follicular maturation was obtained, human chorionic gonadotropin (hCG) was administered and oocyte retrieval was performed about 36 hours later under transvaginal sonographic guidance and general anesthesia. ET was carried out on Day 3 or Day 5 after
oocyte retrieval. Frozen ETs were excluded from the study.
The Embryo Transfer Procedure
We carried out all the ET in the operation theater. Three embryos were usually prepared for transfer. In case, where numbers of embryos formed were less than three, less number of embryos, i.e., one or two were transferred. The patients arrived with semi-filled
bladder in ultrasound-guided group and with empty bladder in clinical touch group. In both clinical touch and ultrasound group, the clinicians started the ET in the same way, i.e., cleaning the external genitalia with a dry swab before insertion of
a sterile speculum into the vagina. The external cervical os was then cleaned with a dry cotton swab and mucus in the cervical canal was removed with a mucus extractor. Embryos were loaded into Wallace sure view and Cook echo tip catheter. The catheter
was then handed over to the clinician who inserted it through the cervical canal. At this stage, there was a difference between the two groups.
In the clinical touch group, when the clinician was satisfied with that he had placed the catheter as close to the fundus as possible without touching it, the plunger was depressed; but in the ultrasound group, the ultrasonographer used a transabdominal
ultrasound to guide the clinician in the positioning of the tip of the catheter to ~15 mm from the fundus of the uterine cavity. The plunger was then depressed and the air bubbles observed to be expelled from the catheter tip. The embryos were injected
over 30 seconds, allowing observation of the movement of the air bubbles into uterine cavity. Removal of the catheter was also monitored by ultrasound and retention of the air bubbles was observed in the fundal position. The catheter was carefully
checked under microscope and the embryo retained within the lumen or adherent to the surface of the catheter were reharvasted. The embryo can be clearly identified by air bubbles inserted on either side, which are seen as bright echoes on the ultrasound
image.
The clinician was then required to rate the ET procedure in terms of ease of transfer before they left the ET room. The rating system guidelines were:
· Very easy: Transfer catheter went straight through the cervix.
· Easy with some difficulty: Required the separation of the transfer catheter to advance the sheath of a stiffer catheter to facilitate the transfer.
· Difficult: Required in tenculum in addition to those requirement in easy category.
A positive pregnancy outcome was a positive blood pregnancy test performed 2 weeks after the ET and an ultrasound scan showing at least one sac in the uterine cavity 2 weeks after the positive pregnancy test. Statistical analysis: A p value <0.05 was
considered to be statistically significant.
Results
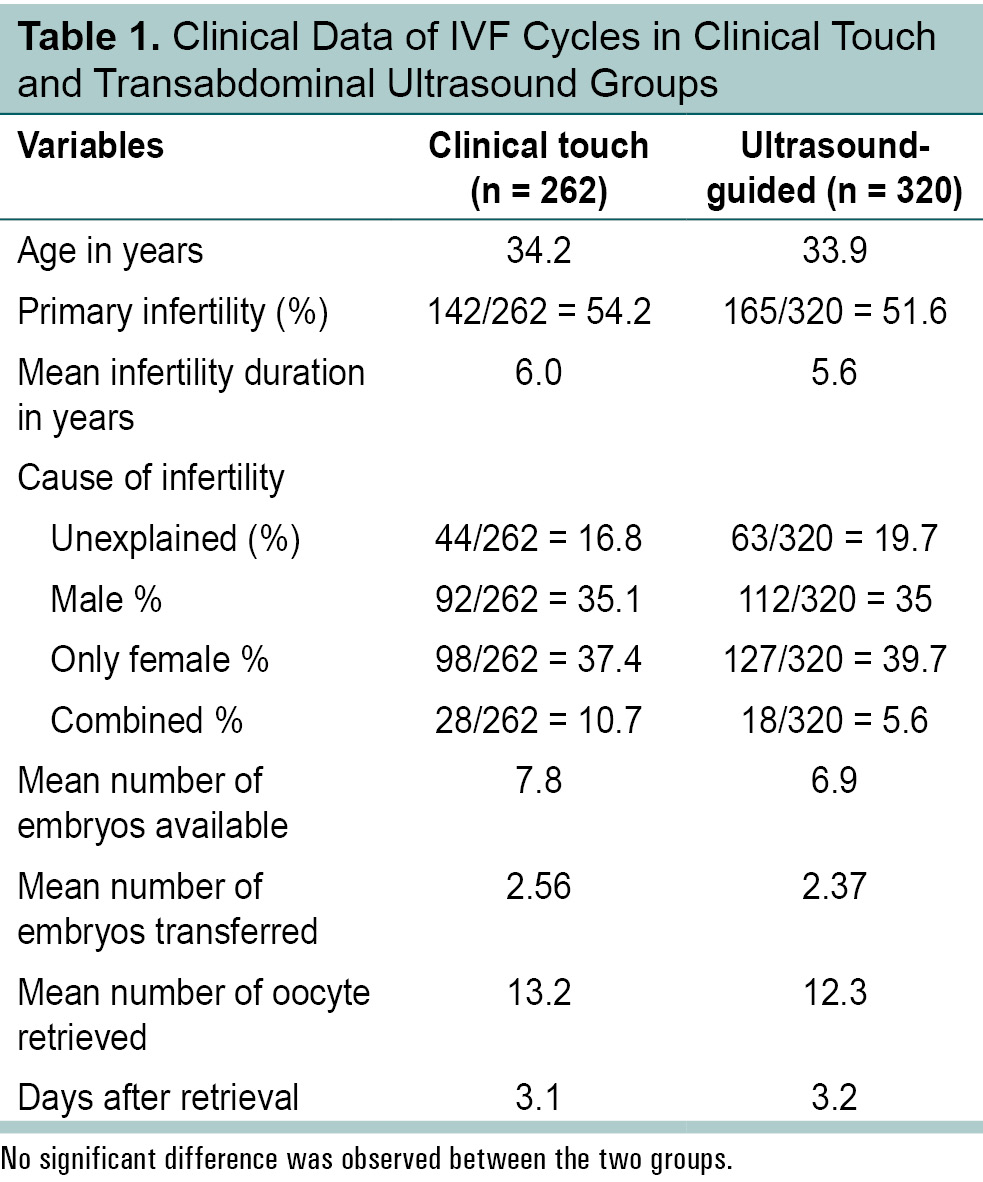
The pregnancy rate and implantation rate appeared higher in the ultrasound-guided group but not significant statistically (Tables 1 and 2).

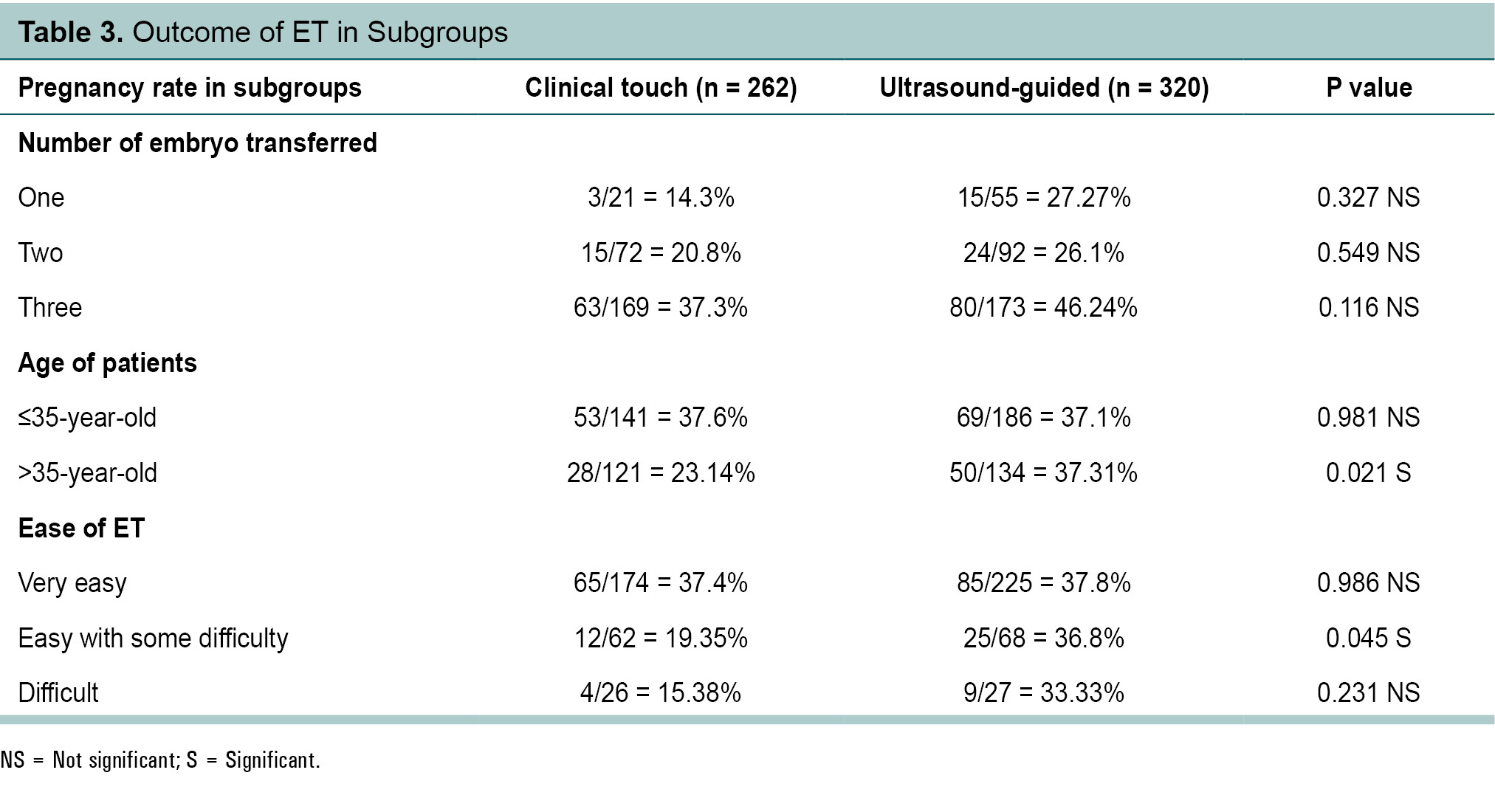
When the analysis was performed controlling for the number of embryos transferred, there was no significant difference in the two groups whether one, two, three embryos were transferred. When controlled for age of women (=35 and >35 years old) again
the results were not significantly different in =35 years of age group but they were statistically significant in age group
>35 years old (23.14% vs. 37.31%, respectively). Pregnancy rate in ‘easy with some difficulty’ ultrasound group was
36.8% vs. 19.35% in comparison to clinical touch group (statistically significant p < 0.05). It may be due to precise recognition of position of uterus in ultrasound-guided cases. If we only examined the cases, which were rated ‘difficult’
the difference in favor of the ultrasound group appeared nonsignificant (Table 3).
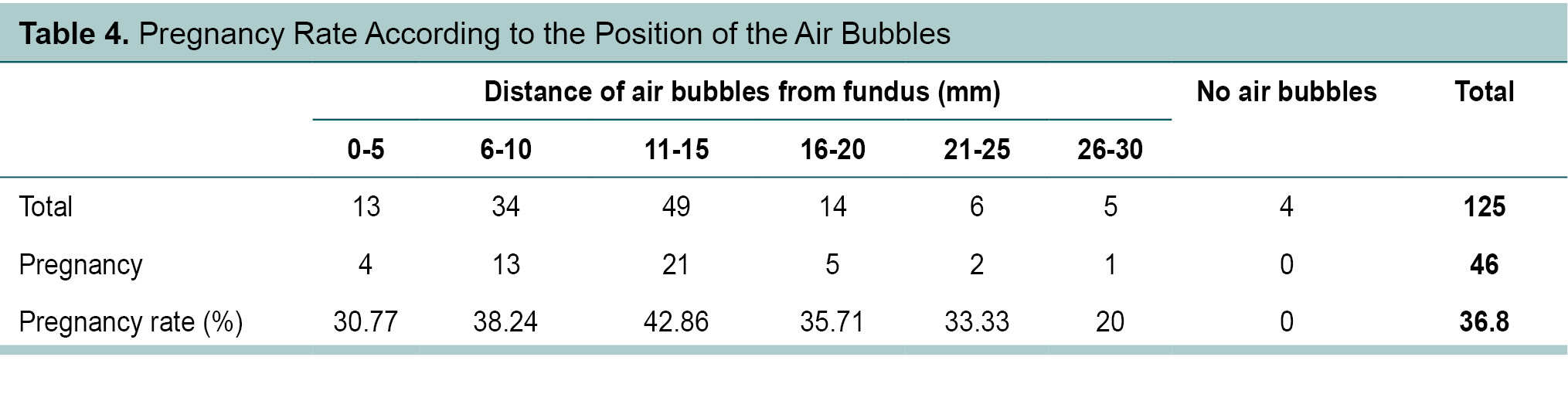
Out of 320 ultrasound-guided ET, in 125 patients, distance of air bubbles from fundus was noted. Pregnancy rate according to the position of the air bubbles was calculated. Maximum pregnancy rate was achieved when the distance of air bubble was between
11-15 mm from the fundus. Four cycles were excluded from this analysis because there was no description of the location of air bubbles in these cases (Table 4).
Discussion
Since the IVF pregnancy was achieved, some aspects of the technique have remained largely unchanged, whilst other have been constantly evolving, the most significant development being in ovulation induction, the use of intracytoplasmic sperm injection
(ICSI) and in the development of culture media. Despite these improvements, the majority of the transferred embryos fail to implant. This failure may be due to poor quality embryo, lack of uterine receptivity or the technique of ET itself9,10.
Defining the factors that are important for successful ET after IVF has been a major issue. Based on the questionnaires distributed amongst highly experienced IVF clinical, Kovacs summarized the answers
11. The factor that got highest votes was the need to remove hydrosalpinx before treatment. The other important factors in order of priority included absence of bleeding, type of catheter used, not touching the fundus, avoid the use
of a tenaculum, removal of all mucus from the cervix, ultrasound details of the cavity before treatment, leaving the catheter in place for at least 1 minute, 30 minutes rest after transfer, dummy transfer before treatment, ultrasonic monitoring of
transfer and antiprostaglandins to prevent contractions. Although the clinician rated the importance of ultrasound guidance as 11th of 12 factors, the role of ultrasound monitoring during transfer should receive more emphasis. The cause of low
priority of this factor might be due to the inconvenience and inaccuracy of transabdominal ultrasound guidance.
Generally, the positions of air bubble indicate the position of the embryos. It was recommended that the tip of the catheter be positioned 15 mm from the fundus of the uterine cavity to avoid placement of embryos close to the uterine fundus7.
In our study, the point of placement of embryo was also 15 mm from the fundal limit of the uterine cavity. We could transfer the embryos to the precise place under transabdominal ultrasound guidance. There was no pregnancy in four cases in which air
bubbles could not be identified. It is likely that these embryos were misplaced probably due to uterine contractions or technical errors. In two cases embryos remained in the lumen of catheter. In other cases, we suppose that the catheter was inadvertently
abutting the internal tubal os and the bubbles disappeared in the tubal canal. Furthermore, we experienced some cases in which the air bubbles moved towards the cornue or the cervix from the position of the tip of the catheter. These observations
also suggest that adequate monitoring by ultrasound guidance is very important during ET.
Evidence emerging from 17 to 20 randomized controlled trials comparing ultrasound guidance versus the ‘clinical touch’ method for ET have been evaluated. Clinical pregnancy rates were found to be statistically significant higher (odd ratio [OR] 1.31-1.50)
with transabdominal ultrasound guidance7,12. It has been reported that high frequency uterine contractions on the day of embryo transfer hinder IVF-embryo transfer outcome13. It was reported that tactile assessment of catheter
placement was unreliable14.
The outer guiding catheter inadvertently abutted the fundal endometrium or the internal tubal os and intended the endometrium. The transfer catheter was seen to be embedded within the endometrium. Transabdominal ultrasound-guided ET can minimize these
endometrial traumas and thus reduce the uterine contractions. As transabdominal ultrasound can supply fine picture of the flexion of the uterus and the curve of the uterine endometrial midline, the clinician can insert the catheter smoothly without
endometrial trauma under the monitoring, and stop the catheter before reaching the fundus. If the curve of the uterine endometrial midline is sharp, we stop the outer sheath before intending the endometrium and advance only the inner catheter, which
is softer than the outer sheath, upto 15 mm from the uterine fundus. These atraumatic procedures probably contributed to successful ET in the present study because bleeding from the endometrium or the uterine cervix is a significant negative factor
for ET, as suggested by Kovacs11.
The procedure was readily accepted by the patients who were reassured by the visualization of the transfer process. The acceptance by the clinician was also high with no significant added time, and the procedure was done with more confidence as the catheter
is advanced to the fundus of the uterus under ultrasound scan guidance. Furthermore, ultrasound-guided ET may have two additional advantages over clinical touch ET when considering that: i) Blind catheter placement has been shown to result in a malposition
of the catheter in >25% of cases, thus indicating that tactile assessment of ET catheter position is unreliable14 and ii) the depth of the embryo replacement into the uterine cavity influences implantation rates, with high pregnancy
rates obtained when the embryos are replaced 15-20 mm from the fundal endometrial surface7. Ultrasound assistance in the ET is a pivotal tool for improving pregnancy rate in assisted reproduction irrespective of whether embryos are
fresh or frozen and replaced in spontaneous, stimulated or artificially prepared cycles. A report showing that ultrasound-guided ET improves outcome in patients with previous failed IVF cycles provides further evidence in this regard12.
Conclusion
There was no significant difference in the pregnancy rate when the number of embryos transferred was controlled. Based on the results obtained from the present study, transabdominal ultrasonography guidance appears to be an essential factor for improving
the results of ET especially in case of easy with some difficulty ET and in older women.
References
-
Al-Shawaf T, Dave R, Harper J, Linehan D, Riley P, Craft I. Transfer of embryos into the uterus: how much do technical factors affect pregnancy rates? J Assist Reprod Genet. 1993;10(1):31-6.
-
Kan AK, Abdalla HI, Gafar AH, Nappi L, Ogunyemi BO, Thomas A, et al. Embryo transfer: ultrasound-guided versus clinical touch. Hum Reprod. 1999;14(5):1259-61.
-
Leong M, Leung C, Tucker M, Wong C, Chan H. Ultrasound-assisted embryo transfer. J In Vitro Fert Embryo Transf. 1986;3(6):383-5.
-
Strickler RC, Christianson C, Crane JP, Curato A, Knight AB, Yang V. Ultrasound guidance for human embryo transfer. Fertil Steril. 1985;43(1):54-61.
-
Lindheim SR, Cohen MA, Sauer MV. Ultrasound guided embryo transfer significantly improves pregnancy rates in women undergoing oocyte donation. Int J Gynaecol Obstet. 1999;66(3):281-4.
-
Wood EG, Batzer FR, Go KJ, Gutmann JN, Corson SL. Ultrasound-guided soft catheter embryo transfers will improve pregnancy rates in in-vitro fertilization. Hum Reprod. 2000;15(1):107-12.
-
Coroleu B, Carreras O, Veiga A, Martell A, Martinez F, Belil I, et al. Embryo transfer under ultrasound guidance improves pregnancy rates after in-vitro fertilization. Hum Reprod. 2000;15(3):616-20.
-
Prapas Y, Prapas N, Hatziparasidou A, Prapa S, Nijs M, Vanderzwalmen P, et al. The echoguide embryo transfer maximizes the IVF results. Acta Eur Fertil. 1995;26(3):113-5.
-
Speirs AL. The changing face of infertility. Am J Obstet Gynecol. 1988;158(6 Pt 1):1390-4.
-
Kojima K, Nomiyama M, Kumamoto T, Matsumoto Y, Iwasaka T. Transvaginal ultrasound-guided embryo transfer improves pregnancy and implantation rates after IVF. Hum Reprod. 2001;16(12):2578-82.
-
Kovacs GT. What factors are important for successful embryo transfer after in-vitro fertilization? Hum Reprod. 1999;14(3):590-2.
-
Anderson RE, Nugent NL, Gregg AT, Nunn SL, Behr BR. Transvaginal ultrasound-guided embryo transfer improves outcome in patients with previous failed in vitro fertilization cycles. Fertil Steril. 2002;77(4):769-75.
-
Fanchin R, Righini C, Olivennes F, Taylor S, de Ziegler D, Frydman R. Uterine contractions at the
time of embryo transfer alter pregnancy rates after in-vitro fertilization. Hum Reprod. 1998;13(7):1968-74.
-
Woolcott R, Stanger J. Potentially important variables identified by transvaginal ultrasound-guided embryo transfer. Hum Reprod. 1997;12(5):963-6.