Expert
Perspectives on Triple Drug Therapy in Type 2 Diabetes Management in India
Abstract
Background: Type 2 diabetes (T2D) is a progressive metabolic disorder that often requires multiple medications to achieve optimal glycemic control. The increasing pill burden and dosing frequency can signi?cantly impact patient adherence,in?uencing
overall treatment e?cacy. This study investigates the perspectives of health care professionals (HCPs) on the use of triple-drug combination therapy—glimepiride, metformin, and sitagliptin—in managing T2D in Indian clinical settings. Method: A nationwide observational survey was conducted between September and December 2024, gathering responses from 214 HCPs across 109 Indian cities. Results: The ?ndings reveal that 86% of HCPs preferred adding an oral agent over initiating insulin
for patients failing dual therapy, with 61.2% supporting triple-drug therapy as a ?rst-line option. Key factors in?uencing the adoption of triple therapy included inadequate glycemic control with dual therapy (79%), presence of comorbidities (53.3%),
and patient a?ordability (28%). E?cacy was ranked as the highest prescribing priority, followed by safety and ease of administration. Most HCPs (96.3%) endorsed triple therapy for working professionals due to its simpli?ed dosing and improved adherence.
Clinical outcomes showed glycemic improvement in more than 50% of patients, with reported adverse e?ects including gastrointestinal discomfort (43.5%) and mild to moderate hypoglycemia (40.7%). Conclusion: These ?ndings highlight the growing
acceptance of triple therapy as an e?ective, patient-friendly approach to diabetes management in real-world practice. The study underscores the importance of balancing e?cacy, safety, and a?ordability to enhance adherence and prevent complications.
Keywords: HCPs, survey, prescribing priority, triple drug therapy, glimepiride, metformin, sitagliptin
Type 2 diabetes (T2D) is a chronic metabolic disorder characterized by defective insulin secretion by pancreatic beta-cells and the inability of insulin-sensitive tissues to respond appropriately to insulin. This requires using different oral and injectable
medications to achieve optimal glycemic control1. Uncontrolled blood glucose levels often require multiple medications2. This situation is further complicated by the presence of comorbidities such as dyslipidemia, hypertension,
and cardiovascular disease, which further increase the overall medication burden3.
An increase in pill burden and dosing frequency have been identified as significant factors contributing to poor adherence. Studies have shown that even in countries with high access to health care, only 39% of patients report good medication adherence4.
This is particularly concerning given the inverse relationship observed between oral antidiabetic drug adherence and glycated hemoglobin (HbA1c) levels. Research has demonstrated that each 10% increase in adherence to oral diabetes medication is associated
with a 0.1% decrease in HbA1c, highlighting the critical role of adherence in achieving glycemic control5.
In light of these challenges, this study aims to investigate the perspectives of the health care professionals (HCPs) on the use of triple-drug therapy combining glimepiride, metformin, and sitagliptin in the management of T2D in India. By focusing on
this specific combination therapy, we seek to understand its impact on glycemic control, potential side effects, and other experiences
of HCPs.
METHODOLOGY
Study Design and Setting
This was an observational survey conducted between September 1 to December 31, 2024, spanning 109 cities across India. The primary objective was to evaluate real-world prescribing practices and clinical perspectives regarding the use of a fixed-dose combination
therapy consisting of glimepiride, metformin, and sitagliptin in the management of type 2 diabetes mellitus (T2DM).
Participants
A total of 222 HCPs—including general physicians, diabetologists, and endocrinologists—actively involved in diabetes care were approached. Electronic informed consent was obtained from all participants; 214 (96.4%) responded to the survey and provided
fully completed and valid responses for analysis.
Survey
The survey utilized an anonymous, structured questionnaire administered through Google Forms™, comprising 25 multiple-choice, closed-ended questions. The questionnaire was initially developed by the research team and subsequently reviewed by a panel of
three diabetes subject matter experts for content accuracy, relevance, and clarity. Modifications based on expert feedback were incorporated prior to dissemination.
RESULTS
A survey of health care providers was conducted across 109 cities in India, with 222 participants, of whom 214 (96.4%) provided complete responses after giving consent.
Eighty-six percent of HCPs preferred adding oral hypoglycemic agents for patients failing dual therapy, while 14% opted for insulin initiation (Fig. 1). Notably, 86% of respondents supported using a triple-drug combination as first-line therapy in newly
diagnosed T2D, while 36% opposed this approach.
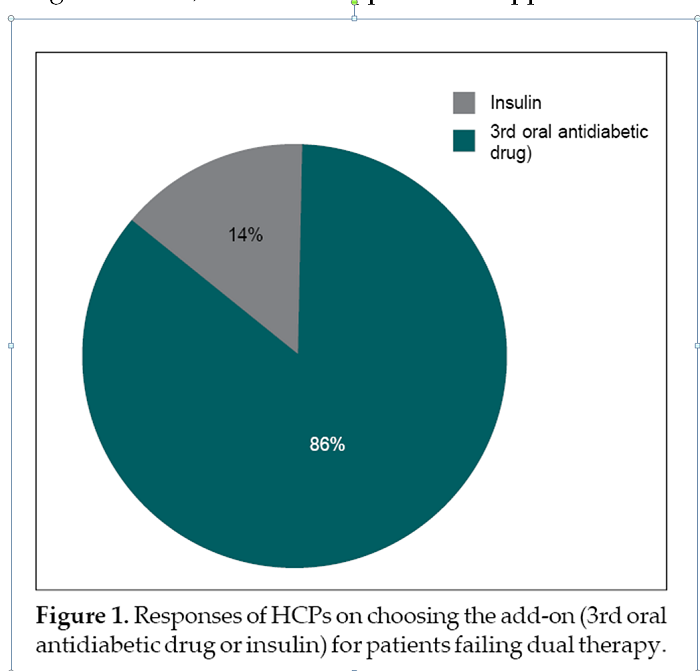
Treatment Strategy Preferences
The primary factors considered when initiating triple therapy included poor control with dual therapy (79%) and monotherapy failure with HbA1c ranging between 8% and 9% (35%). Other factors included the presence of comorbidities (53.3%), duration of diabetes
(24.4%), medication nonadherence (19.2%), poor compliance (31.3%), and treatment costs (28%) (Fig. 2).
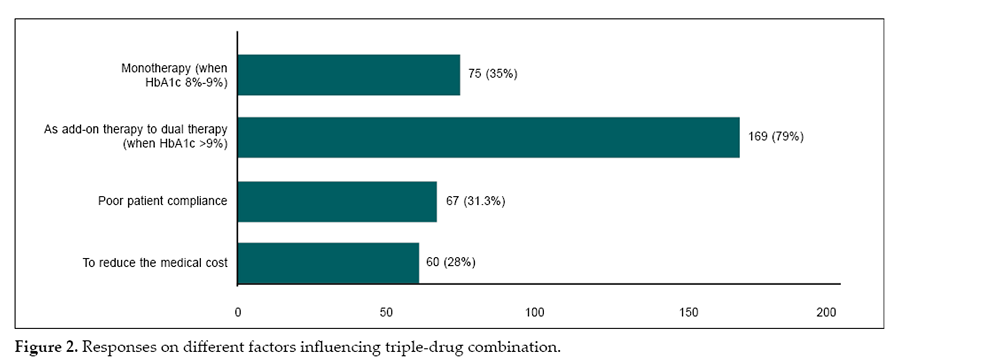
Prescribing Priorities
Health care providers ranked their prescribing consi-derations as follows:
· Efficacy (highest priority, n = 124)
· Safety profile (second priority, n = 114)
· Ease of administration (third priority, n = 117)
· Patient affordability (fourth priority, n = 109).
Clinical Outcomes and Safety
Efficacy: 38.8% of physicians observed glycemic improvement in 25% to 50% of patients and 53.3% of physicians observed improvement in more than 50% of patients.
Adverse effects: The most commonly reported side effects were gastrointestinal issues (43.5%), mild to moderate hypoglycemia (40.7%), and weight gain (8.9%).
Medication timing: 41.1% preferred administration before large meals and 30.4% recommended taking it with large meals.
Patient Education
Health care providers varied in their approach to discussing benefits and risks, with some always addressing them (51.4%), others doing so frequently (21.5%), and a few rarely or never engaging in such discussions (6.5%).
Use of Triple Drug Combination in Working Professionals
Most (96.3%) health care providers considered this combination suitable for working professionals, citing its efficacy and convenient dosing schedule as key advantages.
DISCUSSION
The TRICEPT survey represents a pivotal moment in diabetes management, revealing a significant transformation in the clinical approach. The traditional stepwise treatment model gives way to a more proactive, comprehensive strategy. About 61.2% of physicians
considered a triple-drug combination of glimepiride, metformin, and sitagliptin as first-line therapy, highlighting its efficacy in early diabetes control.
The survey identified efficacy as the top priority when prescribing this combination, with 124 respondents ranking it highest among other factors. This aligns with existing evidence demonstrating the superior glycemic benefits of triple therapy compared
to dual or monotherapy. The ability of the combination to address both fasting and postprandial glucose levels makes it particularly suitable for patients with fluctuating blood glucose patterns. The safety profile also emerged as a critical determinant,
with 114 respondents ranking it second. Common side effects, such as gastrointestinal discomfort (43.5%) and hypoglycemia (40.7%), were reported. These findings highlight the need for close monitoring and individualized dose adjustments, especially
for patients at higher risk of adverse effects.
Interestingly, the survey revealed high acceptability of the triple-drug combination among working professionals, with 96.3% of respondents endorsing its suitability for this group. This underscores its practicality due to reduced pill burden and simplified
administration, which enhance adherence in patients with demanding lifestyles. Affordability was another significant consideration, reflecting the challenge of balancing cost with long-term disease management. With 109 responses, it ranked behind
safety and ease of administration, highlighting its importance in real-world practice, especially in resource-limited settings.
In clinical practice, comorbidities play a significant role in determining the choice of therapy; 53.3% of respondents considered conditions such as cardio-vascular disease and chronic kidney disease while prescribing. These findings emphasize the importance
of holistic management strategies in diabetes care. The relatively low prioritization of disease duration (24.4%) and nonadherence to previous medications (19.2%) suggest that these factors may be secondary to glycemic control and comorbidities in
clinical decision-making. The consideration of comorbidities by 53.3% of respondents as a key factor aligns with the American Diabetes Association (ADA) and European Association Study Diabetes (EASD) consensus recommendations emphasizing consideration
of comorbidity burden in treatment selection6.
The survey results align with existing clinical trials on this combination. Clinical studies, TECOS7 and GRADE8
have demonstrated the efficacy and safety of sitagliptin and glimepiride, particularly when combined with metformin, in achieving durable glycemic control with a manageable side effect profile. The relatively low rates of weight gain (8.9%) reported
in this survey further validate the weight-neutral benefits of sitagliptin and metformin.
CLINICAL IMPLICATIONS
The triple-drug combination significantly simplifies diabetes management by consolidating multiple active ingredients into a single therapy. For patients managing complex medication regimens, especially those with comorbid conditions requiring additional
medications, reducing the pill burden minimizes the cognitive and logistical challenges associated with treatment adherence. This is beneficial for older adults or those with limited health literacy and working professionals, where complex regimens
can lead to unintentional nonadherence.
Patient compliance remains a cornerstone of effective diabetes management. Any barrier in the therapy due to socioeconomic or illiteracy issues can lead to nonadherence9. The simplicity and convenience of a triple-drug combination improve compliance
by reducing the frequency of doses and the complexity of administration. In real-world scenarios, this translates to fewer treatment gaps, reduced health care utilization for managing uncontrolled diabetes, and improved patient satisfaction. Enhanced
compliance also facilitates the health care provider's ability to monitor and adjust therapy based on predictable patterns, improving clinical outcomes.
The combination of glimepiride, metformin, and sitagliptin addresses multiple aspects of metabolic dysfunction in T2D. Glimepiride, a sulfonylurea, enhances insulin secretion, particularly during meals, which helps manage postprandial hyperglycemia
10. Metformin, a biguanide, reduces hepatic glucose production and improves insulin sensitivity, providing robust fasting glucose control
11. Sitagliptin, a dipeptidyl peptidase 4 (DPP-4) inhibitor, augments incretin activity, balancing glucose levels by stimulating insulin release and suppressing glucagon secretion in a glucose-dependent manner12. This synergistic
action provides comprehensive glycemic control, addressing both fasting and postprandial hyperglycemia, a critical factor in preventing fluctuations that increase cardiovascular risk13. Additionally, the weight-neutral and renal-friendly
profiles of sitagliptin and metformin make the combination particularly suitable for patients with obesity, metabolic syndrome, or early-stage chronic kidney disease.
By achieving and maintaining HbA1c targets, triple-drug therapy can prevent or delay the onset of microvascular complications such as retinopathy, nephropathy, and neuropathy14. Moreover, comprehensive glucose control minimizes the risk of
macrovascular complications, including cardiovascular disease, which remains the leading cause of mortality in individuals with diabetes14.
Early and aggressive intervention with this combination can also reduce the long-term health care burden associated with diabetes, including hospitalizations, the need for dialysis or amputation, and other debilitating outcomes. Importantly, triple therapy
provides a bridge to more advanced stages of diabetes care without compromising outcomes.
STRENGTHS AND LIMITATIONS
The study covers a large geographical coverage and sample size, as implemented in Pan-India covering 109 cities with 214 complete responses. The high response rate (96.4%) indicates strong physician engagement. A comprehensive data collection approach
makes the results robust revealing the practical adaptations in clinical settings. One of the limitations includes potential recall bias in reporting adverse events.
Conclusion
This survey provides valuable insights into the real-world implementation of triple therapy with glimepiride, metformin, and sitagliptin in Indian clinical practice. The findings support early consideration of triple therapy in appropriate patients while
highlighting the importance of individualized treatment approaches based on patient characteristics and preferences.
Acknowledgment
We are thankful to Ms BaishaliNath- Manager Medical Department, Ajanta Pharma Ltd and Team Ajanta Pharma Limited for this initiative of TRICEPT.
REFERENCES
1. Galicia-Garcia U, Benito-Vicente A, Jebari S, Larrea-Sebal A, Siddiqi H, Uribe KB, et al. Pathophysiology of type 2 diabetes mellitus. Int J Mol Sci. 2020;21(17):6275.
2. Nathan DM, Buse JB, Davidson MB, Ferrannini E, Holman RR, Sherwin R, et al; American Diabetes Association; European Association for Study of Diabetes. Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation
and adjustment of therapy: a consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2009;32(1):193-203.
3. American Diabetes Association Professional Practice Committee. 10. Cardiovascular Disease and Risk Management: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47(Suppl 1):S179-S218.
4. Tiv M, Viel JF, Mauny F, Eschwège E, Weill A, Fournier C, et al. Medication adherence in type 2 diabetes: The ENTRED study 2007, a French population-based study PLoSOne. 2012;7(3):e32412.
5. Rozenfeld Y, Hunt JS, Plauschinat C, Wong KS. Oral antidiabetic medication adherence and glycemic control in managed care. Am J Manag Care. 2008;14(2):71-5.
6. Davies MJ, Aroda VR, Collins BS, Gabbay RA, Green J, Maruthur NM, et al. Management of hyperglycemia in type 2 diabetes, 2022. A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes
(EASD). Diabetes Care. 2022;45(11):2753-86.
7. Green JB, Bethel MA, Armstrong PW, Buse JB, Engel SS,Garg J, et al; TECOS Study Group. E?ect of sitagliptin on cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2015;373(3):232-42. Erratum in: N Engl J Med. 2015;373(6):586.
8. GRADE Study Research Group; Nathan DM, Lachin JM, Balasubramanyam A, Burch HB, Buse JB, Butera NM, et al. Glycemia reduction in type 2 diabetes - glycemic outcomes. N Engl J Med. 2022;387(12):1063-74.
9. Pourhabibi N, Mohebbi B, Sadeghi R, Shakibazadeh E, Sanjari M, Tol A, et al. Determinants of poor treatment adherence among patients with type 2 diabetes and limited health literacy: a scoping review. J Diabetes Res. 2022;2022:2980250.
10. Basit A, Riaz M, Fawwad A. Glimepiride: evidence-based facts, trends, and observations (GIFTS). [corrected]. Vasc Health Risk Manag. 2012;8:463-72.
11. Hunter RW, Hughey CC, Lantier L, Sundelin EI, Peggie M, Zeqiraj E, et al. Metformin reduces liver glucose production by inhibition of fructose-1-6-bisphosphatase. Nat Med. 2018;24(9):1395-406.
12. Kim JH. E?ects of sitagliptin on insulin and glucagon levels in type 2 diabetes mellitus. Diabetes Metab J. 2015; 39(4):304-6.
13. Zakir M, Ahuja N, Surksha MA, Sachdev R, Kalariya Y, Nasir M, et al. Cardiovascular complications of diabetes :from microvascular to macrovascular pathways. Cureus. 2023;15(9):e45835.
14. Abdul-Ghani M, Puckett C, Abdelgani S, Merovci A, Lavrynenko O, Adams J, et al. Glycemic and non-glycemic benefits of initial triple therapy versus sequential add-on therapy in patients with new-onset diabetes: results from the EDICT study.
BMJ Open Diabetes Res Care. 2025;13(2):e004981.