Abstract
This case report details the management of a
54-year-old male with refractory angina due to in-stent restenosis (ISR) within
a chronic total occlusion (CTO) of the right coronary artery (RCA). Despite
multiple prior percutaneous coronary interventions (PCIs) and maximal
medical therapy, symptoms persisted. Optical coherence tomography (OCT)-guided
PCI, augmented by the Penumbra CAT RX mechanical thromboaspiration system,
revealed heterogeneous neoatherosclerosis and organized thrombus
(Wataru-Yamamoto Type 4 ISR). The sustained negative suction of the Penumbra
device (-29 mmHg), excellent trackability, and maneuverability enabled the
effective debulking of late thrombus, restoring distal flow and OCT clarity.
This facilitated tailored therapy: a drug-eluting stent for fibroatheroma, a
drug-eluting balloon for neointimal hyperplasia, and high-pressure
post-dilation for underexpansion. The case challenges the assumption of the
absence of thrombus in CTOs. It underscores the value of the “P-OCT” protocol
(Prepare with thromboaspiration, Optimize imaging, Characterize pathology,
Treat mechanistically) in ISR-CTO.
Keywords: Penumbra CAT RX, in-stent restenosis, chronic total occlusion, optical
coherence tomography, percutaneous coronary intervention
In-stent
restenosis (ISR) and chronic total occlusions (CTOs) represent complex
challenges in interventional cardiology. ISR, often driven by neointimal
hyperplasia (NIH) or neoatherosclerosis, is compounded in CTOs by fibrocalcific
remodeling and organized thrombus. Traditional angiographic guidance
often fails to accurately delineate the underlying plaque morphology,
resulting in suboptimal stent deployment and a higher incidence of recurrent
events.
Optical
coherence tomography (OCT), with its
high-resolution cross-sectional imaging, has emerged as a critical tool for
characterizing ISR-CTO pathology. However, thrombus remains a persistent
barrier to optimal visualization. The Penumbra CAT RX system1, a
mechanical thromboaspiration device, is traditionally reserved for acute thrombotic lesions.
This
case illustrates its innovative application in a troponin-negative ISR-CTO, integrated with OCT-guided stratification
using the Wataru-Yamamoto classification2, to achieve a
patient-specific therapeutic approach.
CASE
REPORT
A
54-year-old male with a history of hypertension and multivessel coronary artery
disease underwent multiple percutaneous
coronary interventions (PCIs) on the following dates: right coronary artery (RCA) in 2012 and 2019, left anterior descending artery and diagonal bifurcation in 2019, and left circumflex artery in 2019. Despite receiving maximum antianginal therapy—including
isosorbide mononitrate and metoprolol, he experienced 6 months of refractory angina, classified as Canadian Cardiovascular Society Class III.
Diagnostic evaluations revealed T-wave inversions in lead I, aVL,
and V5-V6 on the electrocardiogram, indicating lateral ischemia. A
transthoracic echocardiogram showed severe left ventricular dysfunction, with an ejection fraction of 35%, global hypokinesia, prominent
anterior wall involvement, and Grade I diastolic dysfunction. High-sensitivity
troponin I levels were nondiagnostic at 0.01 ng/mL.
Coronary
angiography revealed a CTO in the RCA, with retrograde collaterals from the
left coronary system. This was classified with a Japanese CTO (J-CTO)3
score of 3 because of factors such as calcification, a blunt stump, and a
bending angle exceeding 45 degrees (Fig. 1).
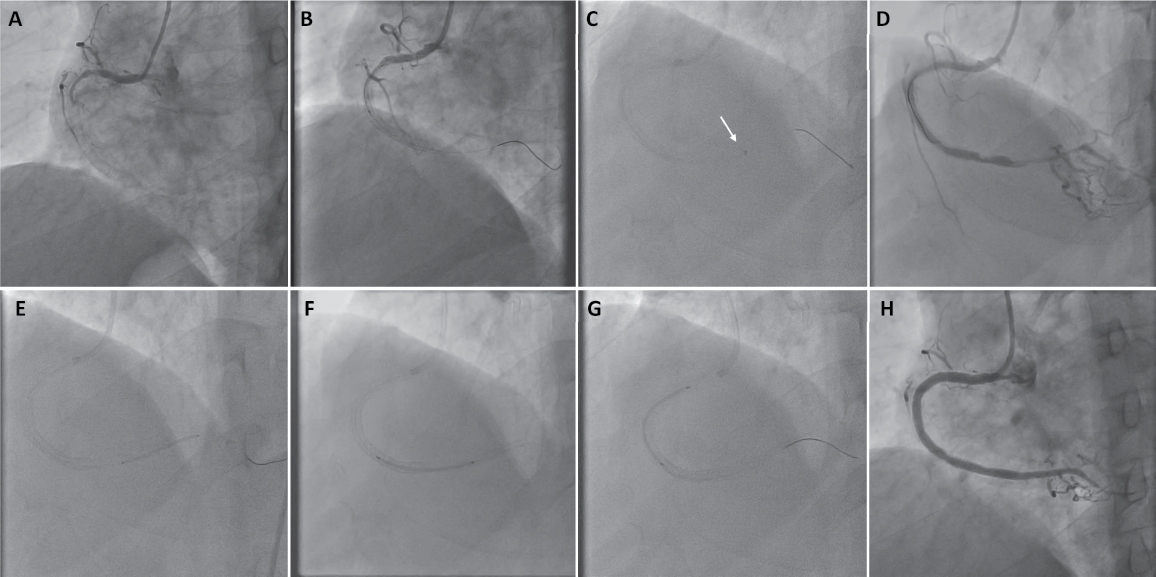
Figure
1. Angiographic images (A to H)
illustrate the procedure as follows: (A) Baseline RCA showing 100%
in-stent restenosis, (B) no-reflow phenomenon following balloon
dilation, (C) Pneumbra-guided thromboaspiration, (D) improved
distal flow, (E & F) drug-eluting stents placement in the distal and
mid segments, (G) drug-eluting balloon treatment in the proximal segment
based on optical coherence tomography findings, and (H) the final
angiographic outcome of the RCA.
The
procedural strategy employed a retrograde approach using a Fielder XT-A wire
and Finecross microcatheter, achieving true lumen re-entry after initial
subintimal tracking. Predilation with a 2.0 mm semi-compliant balloon failed to
restore distal flow (TIMI-1), prompting suspicion of neoatherosclerotic debris
or thrombus.
The 5.3 Fr catheter’s sustained negative suction (-29 mmHg) and
exceptional trackability enabled seamless navigation through the previously stented RCA, aspirating
dense, organized thrombus despite the lesion’s chronicity. Its maneuverability
proved critical in traversing calcified segments, achieving TIMI-2 flow
post-aspiration. Subsequent OCT imaging (Ultreon 2.0) revealed layered,
heterogeneous tissue in the proximal RCA (Wataru-Yamamoto Type 4 ISR) with
invisible struts and neointimal rupture, indicative of organized thrombus. Distally, fibroatheroma with minimal calcification (Gonzalo’s classification: heterogeneous, noncalcified) was identified. Tailored therapy included deployment of
a 3.0 × 28 mm drug-eluting stent (DES) at the fibroatheroma site, application of a 4.0 × 35 mm drug-eluting balloon (DEB) to the NIH-dominant segment, and high-pressure post-dilation with a 4.5 mm noncompliant balloon.
The
final OCT confirmed TIMI-3 flow and a significant increase in the minimum lumen
area from 2.79 to 7.81 mm² (Fig. 2).
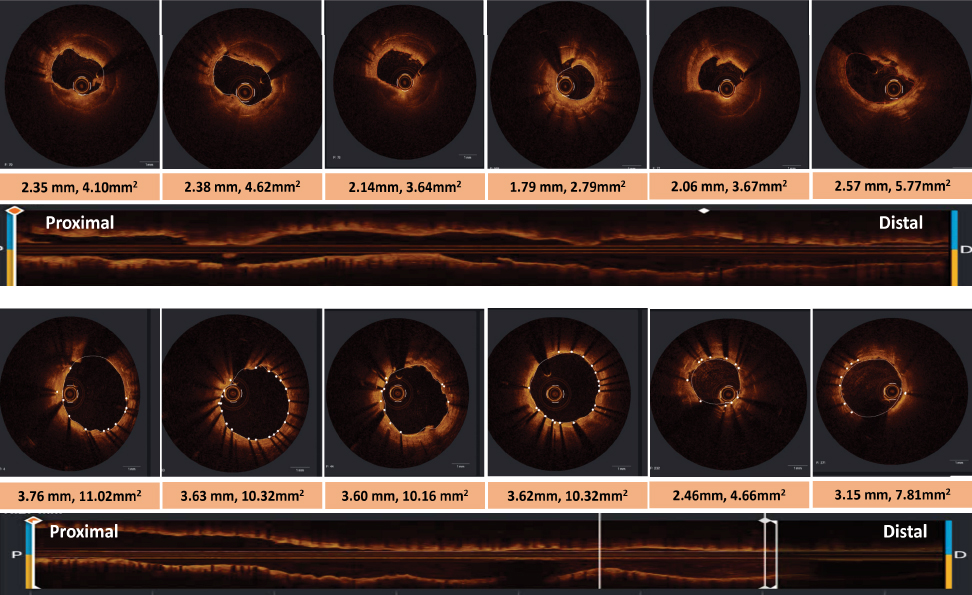
Figure
2. OCT images acquired after
Penumbra-guided thromboaspiration (upper panel) and final OCT images
following stent placement (lower panel).
DISCUSSION
This case challenges the traditional dogma that CTOs lack thrombotic
components. Histopathological studies have demonstrated that ISR-CTOs
frequently harbor organized thrombus beneath layered plaques, driven by chronic
endothelial injury and inflammation. The “Tidy the Tunnel” philosophy—preparing
the lesion with thromboaspiration before OCT—proved pivotal. Thrombus, often
dismissed in CTOs, obscured critical details of neointimal rupture and layered
plaque.
Penumbra’s
aspiration “cleared the path”, enabling OCT to classify the ISR as
Wataru-Yamamoto Type 4 (heterogeneous tissue, invisible struts) and
Gonzalo’s heterogeneous noncalcified plaque, which guided the selection of
DES/DEB. The Wataru-Yamamoto classification, which integrates OCT findings,
provides granular insights into ISR morphology. In this case, Type 4 ISR
(heterogeneous tissue with invisible struts)4 correlated with
prolonged stent duration and thrombotic remnants, necessitating a multifaceted approach
to treatment.
The Penumbra system’s mechanical thromboaspiration uniquely addresses
both soft atheroma and organized thrombus, debulking lesions resistant to
conventional predilation. This contrasts with rheolytic or ultrasound-based
devices, which risk distal embolization in calcified CTOs. Prior studies, such
as the TROFI trial5, have linked residual thrombus to higher rates
of major adverse cardiovascular events (MACE), justifying its use even in
non-acute settings.
OCT-guided stratification further allowed differentiation of
fibroatheroma (targeted with DES) from NIH (treated with DEB), aligning with
the “P-OCT” protocol (Prepare with thromboaspiration, Optimize imaging,
Characterize pathology, Treat mechanistically). This approach aligns with
recent guidelines recommending OCT for stent optimization in complex lesions.
The Wataru-Yamamoto classification2 revealed neointimal
rupture, a feature exclusive to Type 4 ISR—prompting DES deployment.
Conversely, NIH-dominated regions received DEB, avoiding unnecessary stenting. This precision, unattainable angiographically,
underscores the role of OCT in personalizing ISR therapy.
CONCLUSION
This case redefines ISR-CTO management by integrating advanced thromboaspiration
and OCT stratification. The Penumbra CAT RX’s mechanical efficacy
in chronic thrombus debulking, coupled with the Wataru-Yamamoto
classification, enables a shift from blind stenting to pathology-driven
therapy. The “Tidy the Tunnel” approach—preparing the lesion before imaging or
intervention—should be prioritized in complex ISR cases to mitigate under
sizing, residual thrombus, and MACE.
REFERENCES
- Gilchrist IC Jr, Fordham MJ, Pyo R, Reilly JP, Chen O. Mechanical aspiration thrombectomy using the Penumbra CAT RX system for patients presenting with acute coronary syndrome. Cardiovasc Revasc Med. 2022;40S:316-21.
- Yamamoto W, Fujii K, Otsuji S, Takiuchi S, Kakishita M, Ibuki M, et al. Optical coherence tomography characteristics of in-stent restenosis after drug-eluting stent implantation: a novel classification and its clinical significance. Heart Vessels.
2020;35(1):38-45.
- Morino Y, Abe M, Morimoto T, Kimura T, Hayashi Y, Muramatsu T, et al; J-CTO Registry Investigators. Predicting successful guidewire crossing through chronic total occlusion of native coronary lesions within 30 minutes: the J-CTO (Multicenter
CTO Registry in Japan) score as a difficulty grading and time assessment tool. JACC Cardiovasc Interv. 2011;4(2):213-21.
- Mehran R, Dangas G, Abizaid AS, Mintz GS, Lansky AJ, Satler LF, et al. Angiographic patterns of in-stent restenosis: classification and implications for long-term outcome. Circulation. 1999;100(18):1872-8.
- Onuma Y, Thuesen L, van Geuns RJ, van der Ent M, Desch S, Fajadet J, et al; TROFI Investigators. Randomized study to assess the effect of thrombus aspiration on flow area in patients with ST-elevation myocardial infarction: an optical frequency domain imaging study--TROFI trial. Eur Heart J. 2013;34(14):1050-60.